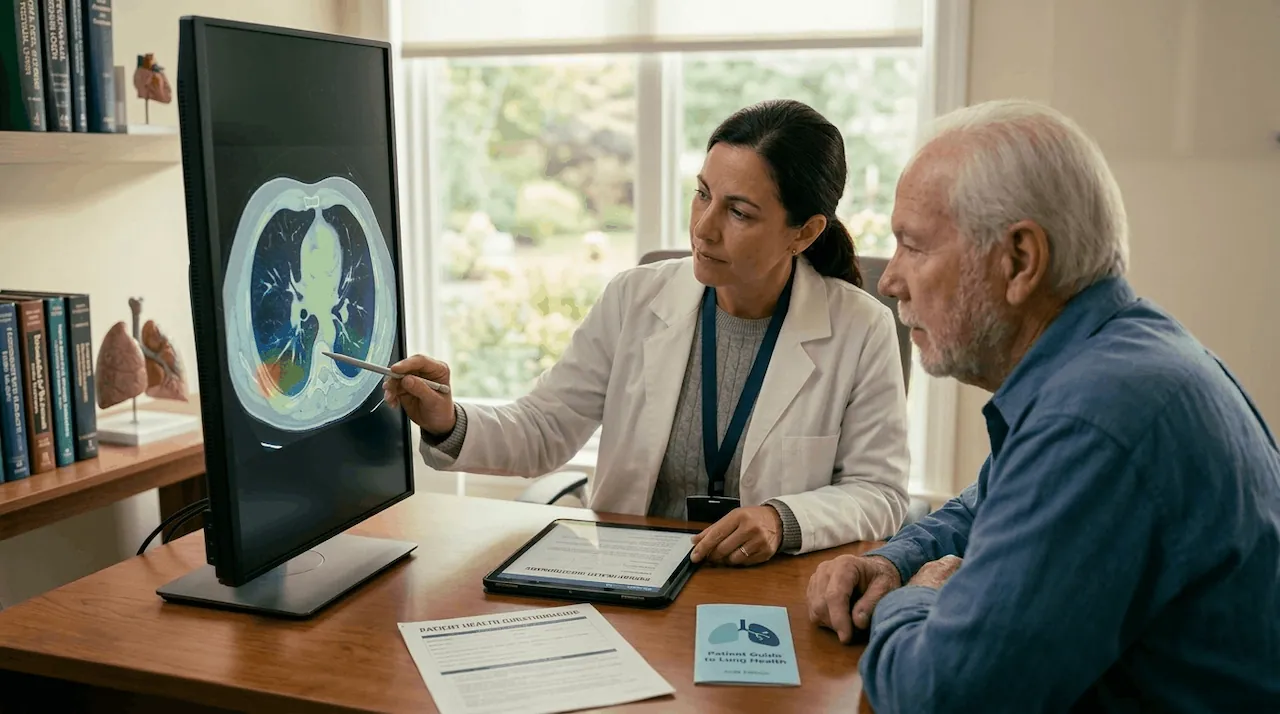
Receiving a clean bill of health after a routine physical should be a relief, but for those who spent decades working in shipyards, construction sites, or industrial plants, a simple “you look fine” often feels incomplete. You know your history. You remember the dust on the job site and the heavy air in the engine room. If you are feeling a persistent cough or a slight heaviness in your chest, the frustration of a standard checkup missing these early signs is real.
Navigating the healthcare system for asbestos-related conditions is different from managing common illnesses. Because this disease often stays hidden for 20 to 50 years, traditional screenings like standard chest X-rays may not catch the subtle changes that matter most. At MesoCare, we act as your guide to help you ask for the specific tests that provide a true roadmap for your health.
If you are ready to move beyond a standard physical, you can learn more about specialized care by visiting our mesothelioma support page.
Understanding Mesothelioma Screening Guidelines 2026
To directly answer the question: How do you screen for mesothelioma? As of 2026, there is no single, universal “standard” screening protocol like a mammogram for breast cancer. Instead, doctors use a high-intent diagnostic toolkit for individuals at increased risk due to asbestos exposure. This protocol typically includes Low-Dose CT (LDCT) scans, biomarker blood tests like SMRP (Soluble Mesothelin-Related Peptides), and a detailed review of occupational history.
You are not alone.
Check your eligibility for financial aid to cover screenings and specialized medical treatments before the 2026 deadlines.
The Reality of Early Detection for Asbestos Diseases
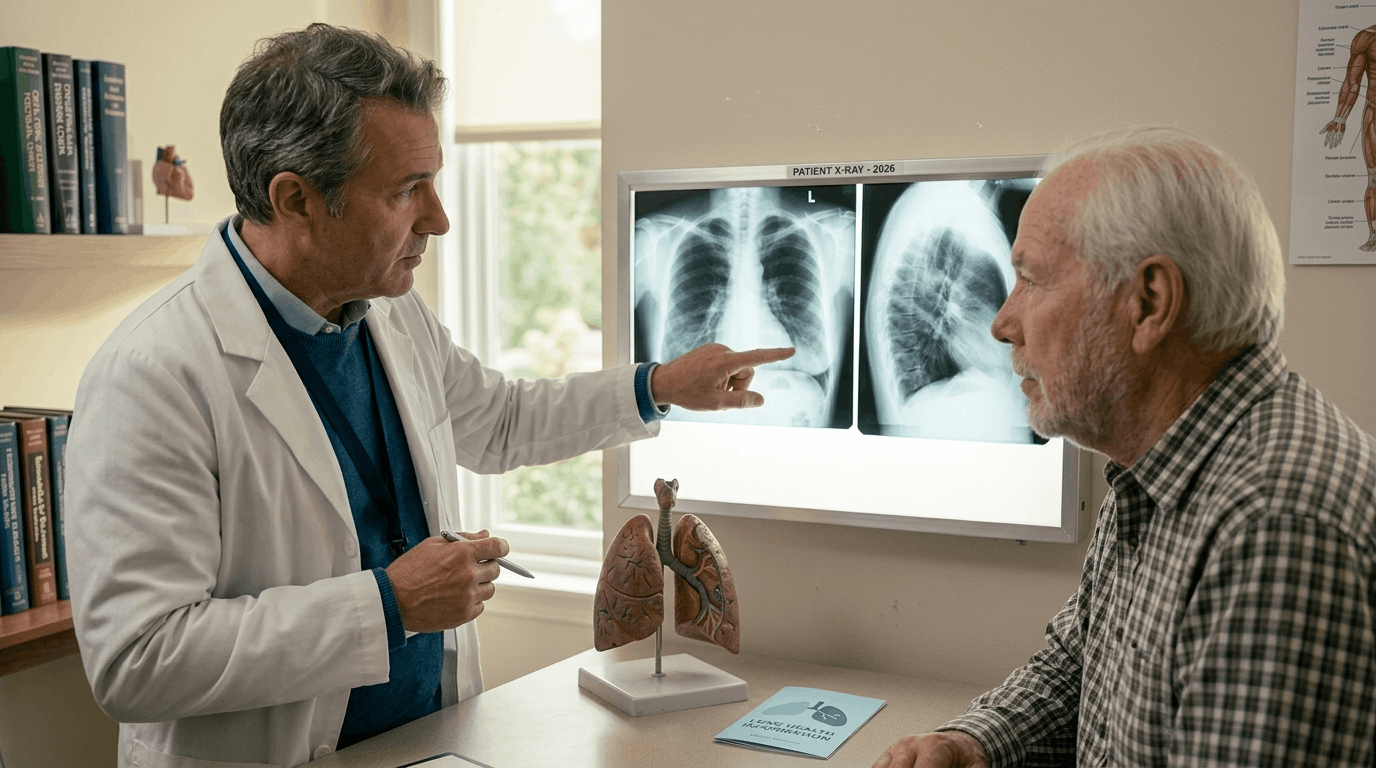
The primary challenge in early detection of asbestos diseases is the latency period. Asbestos fibers are microscopic and needle-like; once inhaled, they lodge into the pleural lining (the mesothelium) and cause chronic inflammation. This process happens in silence for decades. By the time a patient feels a “stitch” in their side or shortness of breath, the disease has often progressed.
Why Standard X-Rays Often Fall Short
In many primary care settings, a chest X-ray is the first tool used. While X-rays are excellent for spotting pneumonia or large tumors, they often miss the early signs of pleural thickening or small fluid buildups known as effusions. For a veteran who worked on Navy vessels, relying solely on an X-ray can lead to a false sense of security. Specialists today recommend more sensitive imaging for those with a documented “high-risk” work history.
“Because the symptoms of mesothelioma such as shortness of breath and chest pain are similar to many other lung conditions, early and accurate diagnosis is critical. Advanced imaging techniques and a thorough review of occupational history are the most effective ways to identify the disease in its earliest, most treatable stages.”
Source: National Institute of Environmental Health Sciences (NIEHS)
The Importance of Occupational History
Your medical history is your most powerful screening tool. Doctors in 2026 are increasingly trained to look at “exposure clusters.” If you spent five years in a shipyard in the 1970s, that single data point is more significant than any current physical symptom. When you meet with a provider, lead with your history. This ensures they prioritize asbestos health monitoring rather than treating you for a common respiratory infection.
The Diagnostic Toolkit: Advanced Scans and Tests
When “preventive maintenance” for your health requires more than a physical, doctors turn to the diagnostic toolkit. These tests are the gold standard for monitoring individuals with a high-risk work history.
Low-Dose CT Scans (LDCT)
Originally used for heavy smokers, LDCT has become the benchmark for mesothelioma screening guidelines 2026. Unlike a standard CT, the LDCT uses about 90% less radiation while still providing a high-resolution, 3D view of the lungs. It is specifically designed to spot small nodules and changes in the pleural lining that occur before a patient feels any symptoms.
The Role of Biomarkers and Blood Tests
The medical community is moving toward non-invasive monitoring using biomarkers. The most common is the MESOMARK® test, which measures SMRPs in the blood. When mesothelial cells become cancerous, they release these proteins at higher levels.
- SMRP (Soluble Mesothelin-Related Peptides): The only FDA-approved biomarker for monitoring.
- Fibulin-3: An emerging marker that helps distinguish between benign asbestos-related changes and actual malignancy.
- Breath Tests: Some clinics are trialing “electronic noses” that detect volatile organic compounds (VOCs) in a patient’s breath.
Pulmonary Function Tests (PFTs)
A PFT is a non-invasive way to measure how much air your lungs can hold and how quickly you can blow it out. While not a “cancer test” itself, it tracks the functional impact of asbestos. If your lung capacity drops over a twelve-month period, it serves as an early warning sign for your doctor to order more intensive imaging.
Caregiver Support: Navigating the Screening Process

For the caregiver, the screening process can be a source of significant “scanxiety.” You are often the one managing the calendar, the insurance calls, and the emotional weight of the results. It is important to remember that screening is about empowerment, not just finding bad news. Catching changes early opens the door to more effective, lung-sparing treatments like pleurectomy and decortication (P&D).
How to Advocate for Your Loved One
If your loved one is hesitant to go to a specialist, remind them that this is not about “looking for trouble”—it is about protecting their future. Use the “earned benefits” language. They worked hard and were exposed to hazards they didn’t ask for; receiving proper medical monitoring is a right they have earned through their years of service.
Veteran Health: Presumptive Conditions and PACT Act Benefits
For the Stoic Veteran, there is good news in 2026. Under the PACT Act, the VA has expanded its “Toxic Exposure Screening” program. This is a 10-minute questionnaire designed to identify service-connected risks quickly. Because mesothelioma is now widely recognized as a “presumptive condition,” veterans who held specific military occupational specialties (MOS) or served on certain ships no longer have to prove their exposure caused their illness—the VA presumes it did.
VA Screening vs. Private Care
Many veterans choose to utilize both systems. While the VA offers excellent “Toxic Exposure Screenings,” private specialists often have access to the very latest clinical trials. At MesoCare, we help you bridge these two worlds, ensuring your VA benefits are documented while you still have access to the best oncologists in the country.
Secondary Exposure: Why Families Should Be Screened
A common misconception is that only the worker is at risk. However, secondary asbestos exposure (also known as take-home exposure) has affected thousands of spouses and children. Fibers carried home on coveralls, hair, and boots can settle in the carpet or laundry room.
Who in the Family Should Be Screened?
If you lived in a household with a high-risk worker before 1980, you should mention this to your doctor. Women, in particular, are frequently diagnosed through secondary exposure after decades of doing a spouse’s laundry. Early detection through LDCT is just as vital for family members as it is for the primary worker.
Accessing Financial Aid for Cancer Screenings and Care
One of the greatest stressors for families is the cost of specialized medical care. A single PET scan or a trip to a top-tier cancer center can be expensive. However, because mesothelioma is uniquely linked to industrial and military exposure, there are resources specifically set aside to help.
Where to find a specialist: Most mesothelioma programs are at one of the 13 NCI-designated cancer centers that run a dedicated mesothelioma service. We list them with phone numbers in our caregiver guide to finding a mesothelioma specialist, including which centers do P/D versus EPP and how to ask for a second opinion.
Asbestos Trust Funds: A $30 Billion Resource
Over 60 companies that manufactured asbestos products have been required by law to set aside billions of dollars in trust funds. These funds are specifically designed to pay for the financial aid for cancer screenings and long-term care. These grants can be used to cover:
- Co-pays for CT and PET scans.
- Travel and lodging for out-of-town specialists.
- Loss of income during the diagnostic phase.
If you need help organizing your records or checking your eligibility for these funds, you can speak with a specialist through our financial assistance guide.
Clinical Fast Fact: Early detection remains the most significant factor in expanding treatment options. Patients diagnosed at an early stage are often eligible for lung-sparing surgeries and advanced clinical trials that can significantly improve long-term outcomes compared to late-stage diagnoses.
Source: American Cancer Society / Mesothelioma Research Update 2026
Navigating a high-risk history is a journey, but you do not have to walk it alone. Whether you are looking for a specialist or simply need to know which screening step to take next, our team is here to provide the roadmap you need. For more resources and patient stories, visit MesoCare.
Medical Disclaimer: MesoCare.org provides educational information and is not a medical provider. We are not doctors. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician with any questions regarding a medical condition. Treatments mentioned are options that may help and should be discussed with a specialist.
Legal Disclaimer: MesoCare.org is a resource center and advocacy group, not a law firm. We do not provide legal advice or guarantee specific financial outcomes. No attorney-client relationship is formed by using this site or contacting an advocate. Potential compensation or grant amounts are estimates and vary by individual case.
