
There is a specific kind of quiet panic that sets in when you cannot catch your breath. For many living with mesothelioma, “breathlessness” or dyspnea is not just a clinical term; it is a daily companion that makes simple tasks like walking to the mailbox or even sitting through a long conversation feel like an uphill climb. If you are a caregiver watching a loved one struggle, the feeling of helplessness can be just as heavy. At MesoCare, we want you to know that while your medical team focuses on the cancer, there are practical, gentle steps you can take right in your living room to reclaim a sense of control over your breathing.
Managing respiratory symptoms is a vital part of your overall mesothelioma symptom management plan. While advanced therapies address the underlying cause, learning mesothelioma breathing exercises can significantly reduce anxiety and physical fatigue. In 2026, healthcare providers are putting more emphasis than ever on “pulmonary rehabilitation” techniques that patients can perform at home to improve their quality of life. This guide will walk you through four foundational exercises designed to expand your lung capacity and calm the nervous system.
Understanding Why Mesothelioma Causes Shortness of Breath
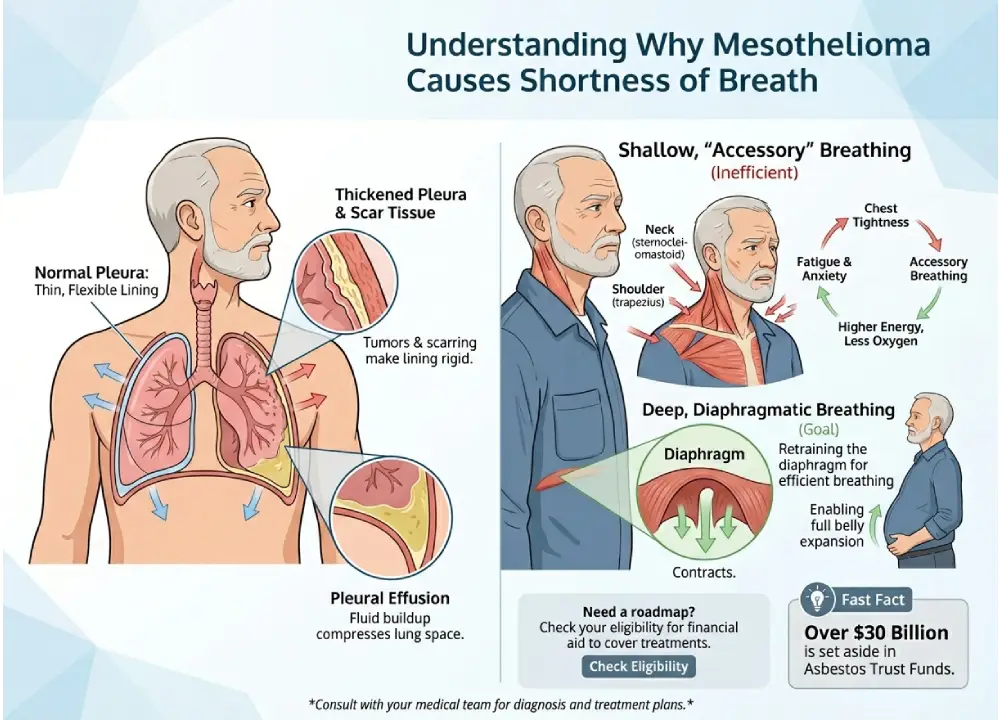
Before we dive into the exercises, it helps to understand what is happening inside the chest cavity. Mesothelioma primarily affects the pleura, which is the thin, lubricated lining around the lungs. As the disease progresses, that lining can thicken or develop scar tissue, making it less flexible. Additionally, many patients experience “pleural effusion,” where fluid builds up in the space between the lungs and the chest wall. This fluid occupies space that the lungs need to expand, leading to that “tight” feeling in the chest.
When your lungs cannot expand fully, your body naturally tries to compensate by taking short, shallow breaths using the muscles in your upper chest, neck, and shoulders. This is known as “accessory breathing.” While it feels like you are working harder to get air, you are actually using more energy and getting less oxygen. This creates a cycle of breathlessness, physical exhaustion, and rising anxiety. The exercises below are designed to break that cycle by retraining your body to use the diaphragm, the large muscle at the base of the lungs specifically built for deep, efficient breathing.
Living with respiratory challenges often means needing extra help at home, specialized equipment, or travel to see top specialists. You are not alone in this. Check your eligibility for financial grants that can help cover the cost of home care, oxygen, and specialized treatments.
1. Pursed Lip Breathing: The “Anchor” for Shortness of Breath
Pursed lip breathing is perhaps the most effective technique for anyone dealing with lung restrictions. It is often the very first thing a physical therapist or a respiratory nurse will teach. The primary benefit of this exercise is that it creates a small amount of back-pressure in your airways, which helps keep them open longer during the exhale. This allows more “trapped” air to leave the lungs, making room for fresh, oxygen-rich air to enter on the next breath.
How to Perform Pursed Lip Breathing
- Relax your neck and shoulder muscles as much as possible. It may help to do this while sitting in a supportive chair.
- Inhale slowly through your nose for a count of two, keeping your mouth closed. It does not have to be a “deep” breath; just a normal, comfortable one.
- Pucker or “purse” your lips as if you were about to whistle or blow out a birthday candle.
- Exhale slowly and gently through your pursed lips for a count of four. The key is to breathe out for twice as long as you breathe in. Do not force the air out; let it escape naturally.
This technique is a lifesaver during physical activity. If you are climbing stairs, walking to the kitchen, or getting up from a chair, try the “exhale on the exertion” rule using pursed lips. By timing your breath with your movement, you prevent the sudden “air hunger” that often causes patients to stop and gasp for air.
“Breathing exercises like pursed lip breathing and diaphragmatic breathing can help you improve your breathing and lung function, especially if you have a condition that makes it hard to breathe.” — Mayo Clinic
2. Diaphragmatic Breathing: Engaging the “Belly” Muscle
Also known as “belly breathing,” diaphragmatic breathing is designed to help you stop using your neck and shoulder muscles to breathe. When you use your diaphragm, you allow the bottom portion of your lungs to fill with air. This is where the most efficient gas exchange happens, meaning you get more oxygen into your bloodstream with every single breath.
Step-by-Step Belly Breathing
- Lie on your back with your knees slightly bent (a pillow under the knees helps), or sit comfortably in a sturdy chair with your back supported.
- Place one hand on your upper chest and the other hand just below your rib cage on your abdomen. This allows you to feel your diaphragm move as you breathe.
- Breathe in slowly through your nose. As you do, focus on making your stomach move out against your hand. The hand on your chest should remain as still as possible.
- Tighten your stomach muscles, letting them fall inward as you exhale through pursed lips. Again, the hand on your upper chest should stay still.
For the “Stoic Veteran” who might find this feels “unnatural” at first, remember that this is how we are born breathing. Watch a sleeping infant, and you will see their belly rise and fall. Relearning this technique reduces the workload on your heart and improves your stamina for daily tasks.
3. Coordinated Breathing: Managing Movement and Breath
Many mesothelioma patients find that they feel perfectly fine while sitting still, but the moment they stand up or reach for something, they lose their breath. Coordinated breathing is a strategy to prevent you from accidentally holding your breath during activity, which is a common habit when we concentrate on a physical task. Holding your breath, even for a few seconds, causes carbon dioxide to build up and oxygen levels to drop, leading to immediate breathlessness.
Practicing Coordination in Daily Life
- Before you start a movement (like standing up from the sofa), take a gentle breath in through your nose.
- While you are doing the “hard part” of the movement (the actual push to stand up), exhale slowly through pursed lips.
- Finish the movement before taking your next breath.
This is an essential tool for maintaining independence. Whether you are lifting a grocery bag, reaching for a dish in a high cabinet, or simply walking across a room, the mantra is “exhale on the effort.” It ensures your oxygen levels stay stable and prevents the sudden spike in heart rate that leads to panic and dizziness.
4. Deep Breathing (Segmental Breathing) for Lung Expansion
Because mesothelioma can cause the lung lining to become rigid, some areas of the lung may not expand as well as others. Deep breathing, or segmental breathing, is a way to encourage specific sections of the lungs to stay active and flexible. It is often used in pulmonary rehabilitation to prevent “atelectasis,” which is when small air sacs in the lungs collapse from disuse.
How to Practice Deep Rib Expansion
- While sitting or standing, place your hands on the sides of your lower rib cage.
- As you breathe in, focus on pushing your ribs outward against the palms of your hands.
- Visualize your lungs expanding like a pair of bellows, filling out to the sides rather than just up toward your collarbone.
- Hold that full breath for just one or two seconds to allow the air to reach the deepest parts of the lung, then perform a slow, controlled exhale through pursed lips.
This exercise helps maintain the mobility of the chest wall. The more flexible your ribs and the muscles between them remain, the easier it is to take a full breath, even if the lung lining itself is thickened. Think of it as “stretching” your lungs from the inside out.
The Connection Between Anxiety and Breathing
It is important to acknowledge the “breathlessness-anxiety cycle.” When you feel short of breath, your brain sends a “danger” signal. This causes your heart rate to increase and your breathing to become even shallower and faster. This, in turn, makes the shortness of breath worse. It is a frightening loop that can lead to a full panic attack.
By using these exercises, you are doing more than just moving air; you are sending a signal back to your brain that says, “I am in control. We are safe.” The mechanical act of slow, pursed-lip breathing actually stimulates the vagus nerve, which triggers the body’s parasympathetic nervous system (the “rest and digest” mode). For the Caregiver, being able to quietly coach a loved one through these steps provides a tangible, practical way to help when things feel out of hand. Instead of saying “just relax,” you can say, “Let’s do three pursed-lip breaths together.”
When to Talk to Your Patient Advocate or Doctor
While home exercises are incredibly helpful, they are one piece of a larger care plan. If you notice that your shortness of breath is changing rapidly or feels different than usual, it is time to seek professional guidance. Indicators that you may need additional medical support or a change in your cancer treatment strategy include:
- Sudden, sharp chest pain that gets worse when you take a deep breath.
- A new or worsening cough that produces yellow, green, or blood-tinged phlegm.
- Feeling significantly breathless even while sitting perfectly still for long periods.
- Needing to sleep propped up on three or four pillows just to be able to breathe comfortably at night.
- Swelling in your ankles or legs, which can sometimes be related to how the heart and lungs are working together.
In many cases, these symptoms can be addressed through simple procedures like a thoracentesis (draining fluid) or adjusting your supportive medications. Never feel like you are “bothering” your medical team by reporting these changes. Managing your comfort and “breathability” is just as important as the treatments targeting the cancer itself.
Practical Tips for a Breath-Friendly Home
In addition to exercises, simple environmental changes can reduce the strain on your lungs. At MesoCare, we suggest these adjustments to your daily routine:
- Use a Handheld Fan: Research shows that a cool breeze from a small fan directed at the face can trick the brain into feeling like it’s getting more air, instantly reducing the sensation of breathlessness.
- Cool the Air: Humid, heavy air is harder to process. Keep your home at a comfortable, slightly cool temperature.
- Steam for Congestion: If you feel “congested,” a warm shower or a bowl of steaming water can help loosen mucus, making your exercises more effective.
- Fragrance-Free Zone: Avoid strong perfumes, scented candles, or harsh cleaning chemicals that can irritate sensitive airways.
By combining a breath-friendly environment with daily exercise, you create a foundation of support that allows you to focus on living your life, rather than just managing a diagnosis.
If you find that performing these exercises makes you feel dizzy, stop immediately and return to your normal breathing pattern. It is always best to perform these while sitting down until you are confident in how your body reacts. As your stamina improves, you might find that you can walk further or engage more in family gatherings without the constant fear of losing your breath.
Support for the Path Ahead

We know that every breath counts. Whether you are a Navy veteran who spent years in a boiler room or a daughter managing her father’s daily care, your comfort is a priority. These exercises aren’t just “homework”, they are a way to take a small piece of your power back from a difficult diagnosis. At MesoCare, we are dedicated to connecting you with the medical experts, pulmonary specialists, and financial resources that make this journey easier to navigate. You don’t have to catch your breath alone.
Fast Fact: The Impact of Breathing Retraining
Clinical studies indicate that up to 90% of pleural mesothelioma patients experience shortness of breath. However, patients who consistently practice pursed-lip and diaphragmatic breathing report a 30% reduction in the “perceived distress” of breathlessness, leading to better sleep and increased physical activity. (Source: Journal of Clinical Medicine)
Medical Disclaimer: MesoCare.org provides educational information and is not a medical provider. We are not doctors. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician with any questions regarding a medical condition. Treatments mentioned are options that may help and should be discussed with a specialist.
Legal Disclaimer: MesoCare.org is a resource center and advocacy group, not a law firm. We do not provide legal advice or guarantee specific financial outcomes. No attorney-client relationship is formed by using this site or contacting an advocate. Potential compensation or grant amounts are estimates and vary by individual case.
